Mumps Makes an Unwelcome Comeback in Hawaii
What was thought to be an ancient disease has made an unwelcome comeback in Hawaii over the last few years.
Mumps, a disease marked by swollen and painful salivary glands on one or both sides of a person’s face, continues to circulate the Hawaiian island chain, with more than 900 confirmed cases of mumps infection statewide as of March 2018.
The Hawaii State Department of Health (DOH) has reported cases of the disease in children and adults, both vaccinated and unvaccinated, with nearly 60 percent appearing in adults aged 18 years and older.
“We do not know the cause of the recent mumps outbreak, but there are several factors that could contribute to it,” says Dr. Douglas Kwock, a pediatrician and chief medical officer of Pali Momi Medical Center.
“While receiving two doses of the mumps vaccine is the best way to protect yourself from infection, two doses of mumps vaccine only achieves about 88 percent protection," explains Kwock, who completed his pediatric residency at Duke University and his fellowship in pediatric infectious disease at Stanford University.
"Secondly," Kwock continues, "as the mumps virus is easily spread through contact with respiratory secretions or saliva from an infected person via coughing and sneezing, if infected individuals are not avoiding contact with others by staying home, then the virus continues to spread in the community.”

Signs and symptoms of mumps usually appear within two to three weeks after exposure to the virus. In addition to parotitis (swelling of the salivary glands), they include the following:
- Fever.
- Headache.
- Muscle aches.
- Weakness and fatigue.
- Loss of appetite.
- Pain while chewing or swallowing.
“More severe complications of mumps include orchitis, an infection in the testes that can cause sterility; ooporitis, an infection in the ovaries; and pancreatitis, deafness, meningitis and encephalitis,” Kwock says.
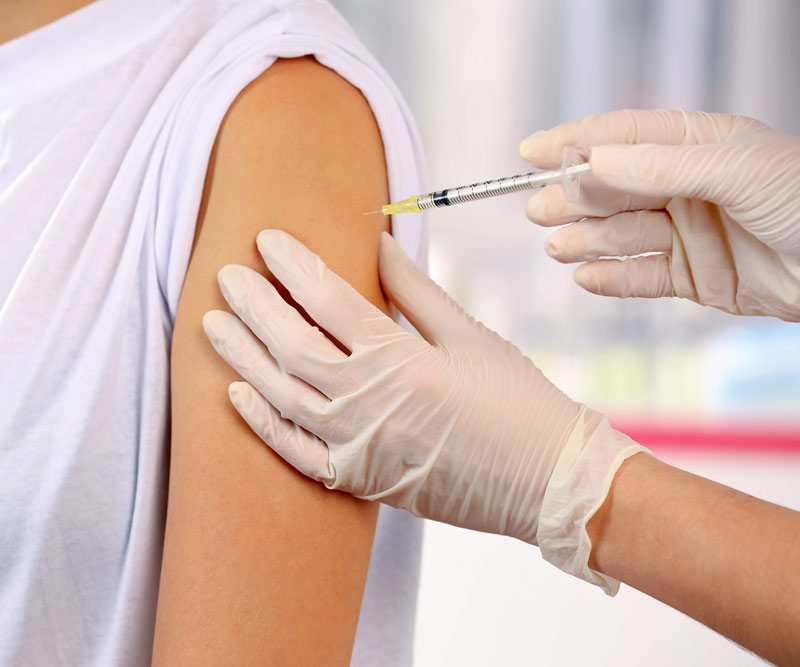
According to Kwock, the best way to prevent mumps is to get vaccinated.
The MMR vaccine protects against not only mumps, but two other infectious diseases – measles and rubella.
In addition to the routine MMR vaccine recommendations, during an outbreak, the DOH recommends adolescents ages 10-19 years and adults born in 1957 and later should receive an additional MMR vaccine dose, regardless of previous age-appropriate vaccination or documentation of a blood test showing immunity to mumps.
MMR vaccine doses should be separated by at least four weeks. An individual should receive no more than three doses of mumps-containing vaccine.
If you suspect or are diagnosed with mumps, you should self-isolate and avoid exposure to others for nine days after onset of parotitis.
Those who have been exposed to mumps and are not vaccinated should not attend school, work or travel from day 12 through day 25 after exposure.
“During a ‘mumps outbreak,’ adhere to DOH recommendations on receiving a third mumps ‘outbreak’ vaccine dose, stay home if you have mumps symptoms, and wash your hands,” Kwock says.
**Health care providers should report any suspected cases of mumps to the DOH immediately by calling the disease reporting line at 808-586-4586.
Published on: March 19, 2018